2025
/in impressionen - 2025/by Kinderwunschpraxis edv
Lio

Theo





Hannah


Nael William







Josephina

Lelliana Videl
Dank eurer Hilfe durften wir noch einmal ein kleines Wunder erleben und können jetzt unser 2tes Kind im Arm halten.
Vielen Dank für die wundervolle und herzliche Behandlung, wir haben uns bei euch immer sehr wohl gefühlt.



Isabella Jola

Levi Amaro

Jule Corinna

Leon



Leni


Yuna



Lilly Vaiana

Kara

Benjamin

Mailo
Wir möchten uns ganz herzlich beim ganzen Team für die tolle Unterstützung und Begleitung während der Behandlung bedanken.

Wir sind sehr froh und dankbar dafür, dass sowohl die Schwangerschaft, als auch letztendlich die Geburt so gut verlaufen sind und wir unseren kleinen Mann in Händen halten dürfen. Dank Ihnen ist es erst so weit gekommen! Merci nochmals!

Emilia


Tara

Paul Jakob

Alara


Donna


Leon


Matthias


Julia


Nora

Caya Elsa Jlvi
Haylee Malia

Laura

Milan


Anna

Frederik

Dimitrije

Aurora

Milian

Elea

Dorina


Blastozystenkultur/ Erweiterte Kultur
/in Blastozystenkultur/ Erweiterte Kultur/by Kinderwunschpraxis edvBei der Kultivierung befruchteter Eizellen sind in den letzten Jahren deutliche Fortschritte erzielt worden. Soweit möglich versuchen wir mehrere befruchtete Eizellen weiter zu kultivieren und den Embryotransfer erst am Tag 5 nach Eizellentnahme im Blastozystenstadium vorzunehmen. Bei der Entwicklung bis zum Blastozystenstadium kommt es bei ca. 60% der befruchteten Eizellen zu einem Entwicklungsstopp. Diese natürliche Selektion während der Kultur führt dazu, dass oftmals nur 1 bis 2 wirklich gut entwickelte Embryonen das Blastozystenstadium erreichen.
Unser Ziel ist der single-embryo-transfer, also der Transfer eines gut entwicklungsfähigen Embryos, um möglichst eine Einlingsschwangerschaft zu erzielen. Überzählige Embryonen können ebenfalls kryokonserviert werden.
Blastozystenkultur
/in Blastozystenkultur/by Kinderwunschpraxis edvBei der Kultivierung befruchteter Eizellen sind in den letzten Jahren deutliche Fortschritte erzielt worden. Soweit möglich versuchen wir mehrere befruchtete Eizellen weiter zu kultivieren und den Embryotransfer erst am Tag 5 nach Eizellentnahme im Blastozystenstadium vorzunehmen. Bei der Entwicklung bis zum Blastozystenstadium kommt es bei ca. 60% der befruchteten Eizellen zu einem Entwicklungsstopp. Diese natürliche Selektion während der Kultur führt dazu, dass oftmals nur 1 bis 2 wirklich gut entwickelte Embryonen das Blastozystenstadium erreichen.
Unser Ziel ist der single-embryo-transfer, also der Transfer eines gut entwicklungsfähigen Embryos, um möglichst eine Einlingsschwangerschaft zu erzielen. Überzählige Embryonen können ebenfalls kryokonserviert werden.
ICSI Therapie
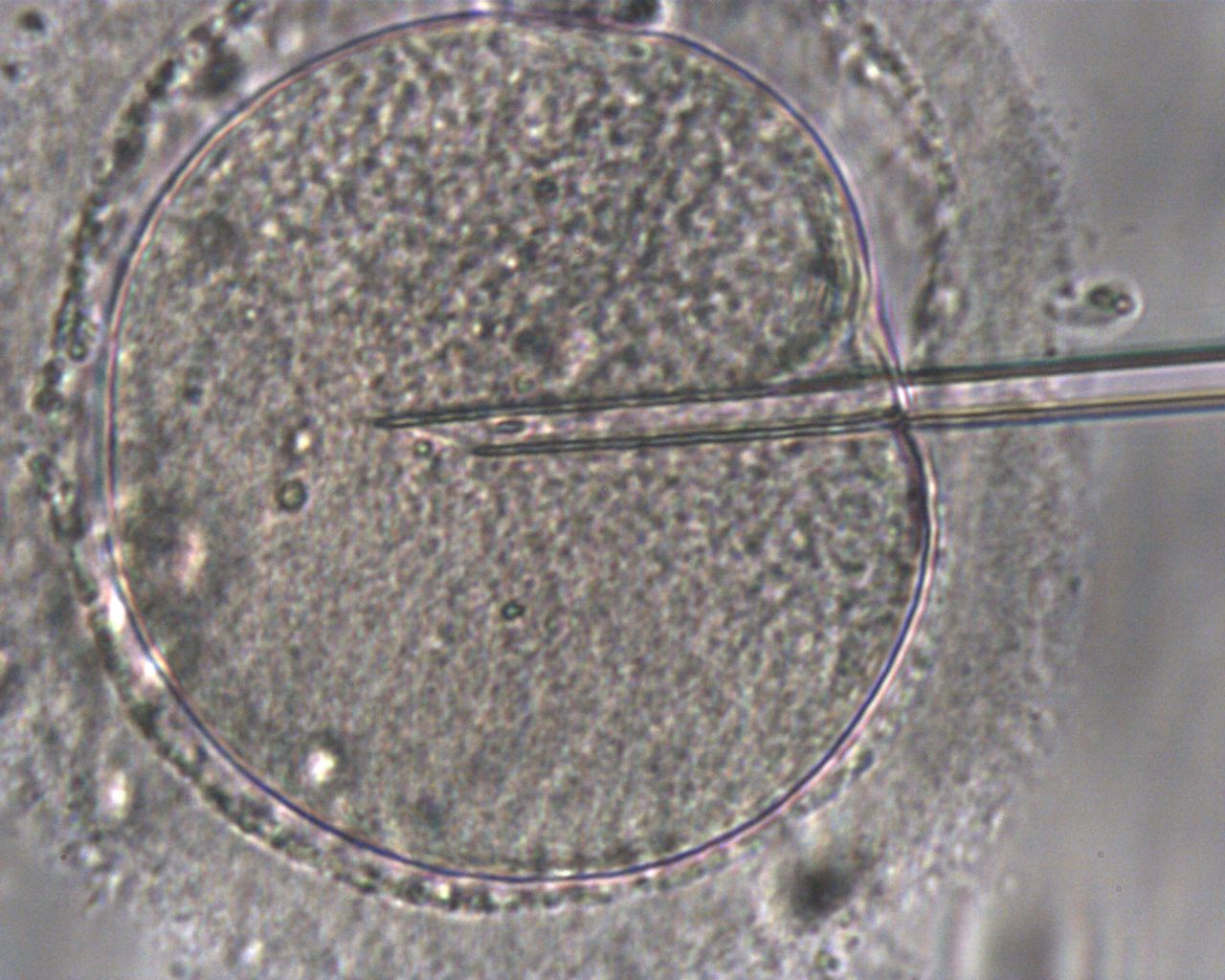
/in ICSI (Intracytoplasmatische Spermieninjektion)/by econsorDie ICSI (Intrazytoplasmatische Spermieninjektion) ist eine spezielle Methode der In-vitro-Fertilisation. Sie wird eingesetzt, wenn eine schwere Störung der Spermienqualität vorliegt (siehe Spermientest). In diesem Fall geht man davon aus, dass die Spermien nicht in der Lage sind, aus eigener Kraft in die Eizelle einzudringen. Bei der herkömmlichen IVF-Behandlung, bei der Eizellen und Spermien lediglich in einer Kulturschale zusammengebracht werden, käme es daher nicht zu einer Befruchtung. Bei der ICSI-Therapie wird daher in jede reife Eizelle ein einzelnes Spermium des Partners injiziert. Dazu wird die Eizelle unter ein Mikroskop gelegt, mit einer Glaskapillare angesaugt und festgehalten. Anschließend wird ein gut bewegliches Spermium durch eine zweite dünne Glaskapillare hochgezogen und direkt in die Eizelle eingebracht. ICSI ist also ein zusätzliches Verfahren im Labor, aber für die Patientin sind die Behandlungsschritte identisch mit der IVF-Therapie.
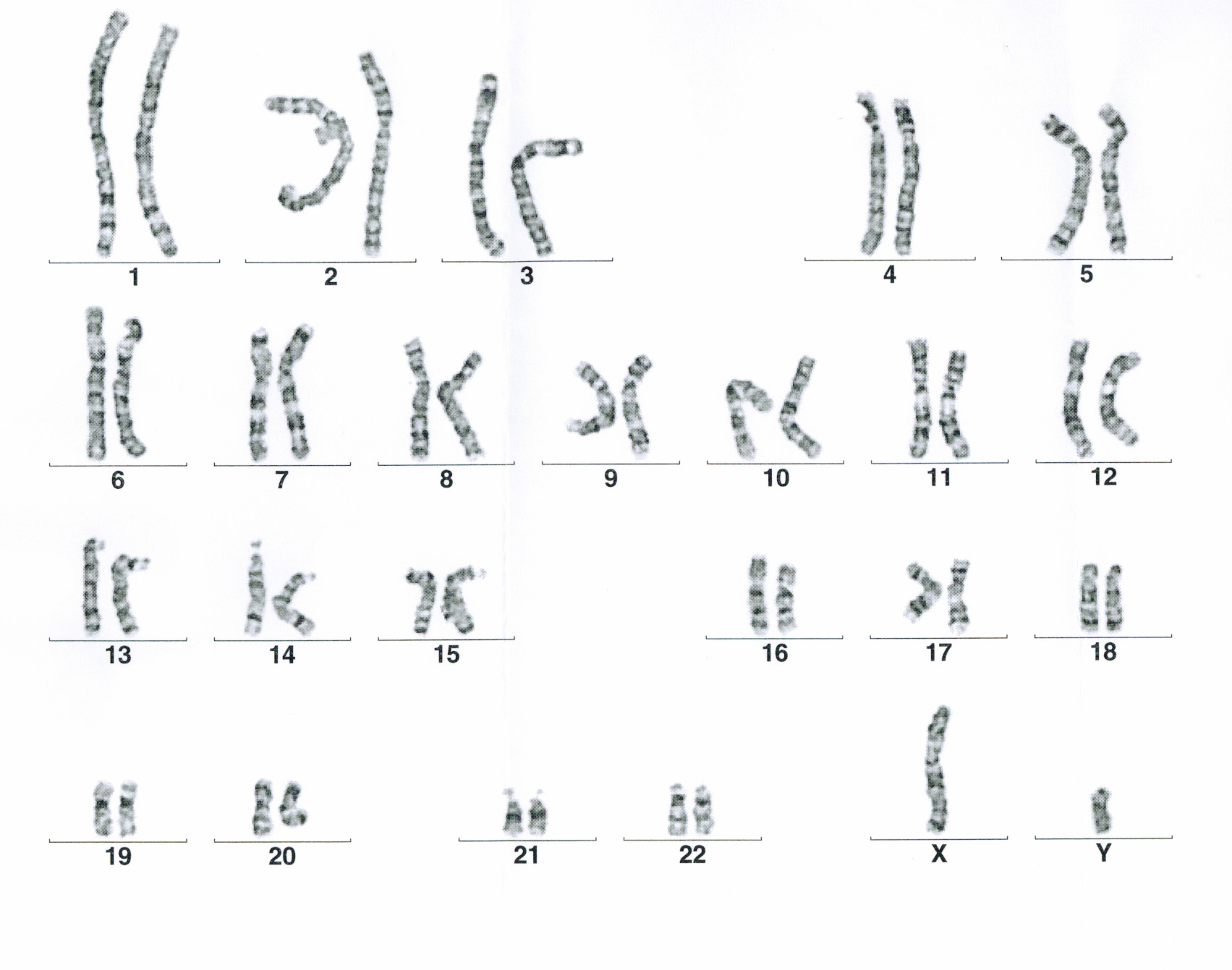
Vor Beginn der Therapie muss geklärt werden, ob eine konventionelle IVF oder eine ICSI notwendig ist. Der entsprechende Antrag auf Kostenübernahme kann bei Ihrer Krankenkasse gestellt werden. Diesen Antrag erhalten Sie von uns, nachdem wir Ihnen in einem Beratungsgespräch die Kosten- und Versicherungssituation erläutert haben. Für die ICSI-Therapie sind zwei Spermiogramme im Abstand von 12 Wochen erforderlich, die den Kriterien der Krankenkassen entsprechen. Es kann daher sein, dass nach dem Erstgespräch ein weiteres Spermiogramm erforderlich ist. Zusätzlich wird eine Chromosomenanalyse bei beiden Partnern empfohlen. In den neuen Richtlinien zur künstlichen Befruchtung 2017 ist festgelegt, dass Männer vor einer ICSI-Therapie von einem andrologisch qualifizierten Arzt untersucht werden müssen.
Special diagnostics for repeated miscarriages or implantation failures
/in Special diagnostics/by econsorMiscarriages occur in 11-15% of all pregnancies. The percentage will increase continuously with women´s age reaching 50% once the women´s are past age 45. The reason for this are randomly occurring chromosomal defects, which can not be treated. However, if there are 3 or more consecutive miscarriages it is referred to as abitual abortions. This concerns 1% of all pregnancies. In some of the patients defects can be defected that can be treated, so further examinations may be useful.
- Hysteroscopy – to exclude malformations of the uterus
- Blood sample for chromosomal analysis – to exclude congenital genetic defects
- Blood sample for hormone analysis -to exclude hormonal causes (eg thyroid gland malfunction)
- Blood sample to exlude imbalance of clotting factors and antibodies as a cause
- Biopsy of the endometrium (the lining of the uterus) for immunohistological examination for uterine killer cells or plasma cells as a sign of inflammation
In some patients with recurrent miscarriage or implantation failure, treatable disorders can be diagnosed. A biopsy of the endometirum (the lining of the
uterus) may be taken for immunohistological examination for uterine killer cells or plasma cells, which can be a sign of inflammation.
Hysteroscopy
/in Hysteroscopy/by econsorFor a hysteroscopy, a long, approximately 3mm thin camera instrument (hysteroscope) is inserted into the uterine cavity, and saline solution is flushed through this, so that the uterine cavity unfolds.
The interior of the uterus with the opening to the fallopian tubes can then be seen on the monitor and abnormalities can be detected. The examination takes a
few minutes and is performed in the first half of the menstrual cycle. It is offered in our practice (with or without anesthesia).
Malformations of the uterus that exist since birth (for example a septum in the uterus) can be removed surgically. Also fibroids and cluttering of the endometrium can interfere with pregnancy and would need to be removed before starting therapy.
Fallopian Tube Patency
/in Fallopian Tube Patency/by econsorThere are different methods used to check the patency of the fallopian tubes. One option is a laparoscopy with tubal patency testing (chromopertubation). With the help of a catheter, coloured fluid is injected via the uterus into the fallopian tubes, which then passes into the free abdominal cavity, and can be observed directly with a camera during the laparoscopy. The procedure is performed under general anasthesia, but usually on an outpatient basis, which means that you can leave the clinic again on the same day. This method provides the most reliable information about the condition oft he fallopian tubes and is especially recommended for patients with previous operations or after abdominal

Es gibt verschiedene Methoden, die Durchgängigkeit der Eileiter zu prüfen. Eine Möglichkeit ist eine Bauchspiegelung mit Eileiterdurchgängigkeitsprüfung (Chromopertubation). Mit Hilfe eines Katheters wird farbige Flüssigkeit durch die Gebärmutter in die Eileiter gespritzt, die anschließend in die freie Bauchhöhle
inflammation.
The least invasive method (also without anasthesia) to check tubal patency is by sonography (ultrasound). Since the fallopian tubes cannot normally be visualized by sonography, a harmless solution (foam ExEm® Foam Kit) is introduced into the uterus via a small plastic catheter. This foam produces a quick and easy expansion of the fallopian tube walls, which can be seen on the ultrasound image. This examination is performed in our practice and is particularly suitable for patients without previous gynecological disease.

Menstrual cycle monitoring
/in Menstrual cycle monitoring/by econsorThe purpose of cycle monitoring is to determine whether you have an ovarian follicle, ovulation and corpus luteum formation. Normally, an egg cell grows in the follicle every month. After ovulation, the egg cell enters the fallopian tube and is fertilised by a sperm. Only four days later does the fertilised egg arrive in the uterus and implant in the uterine lining. During the first weeks of pregnancy, the corpus luteum, which is formed on the ovary from the ruptured follicle, produces the hormone progesterone to support pregnancy. Women with regular, approximately 28-day cycles, are generally expected to have unremarkable cycles when monitored. Women who have a prolonged cycle, irregular bleeding or the first signs of menopause, should have their follicle growth checked if they wish to have children.
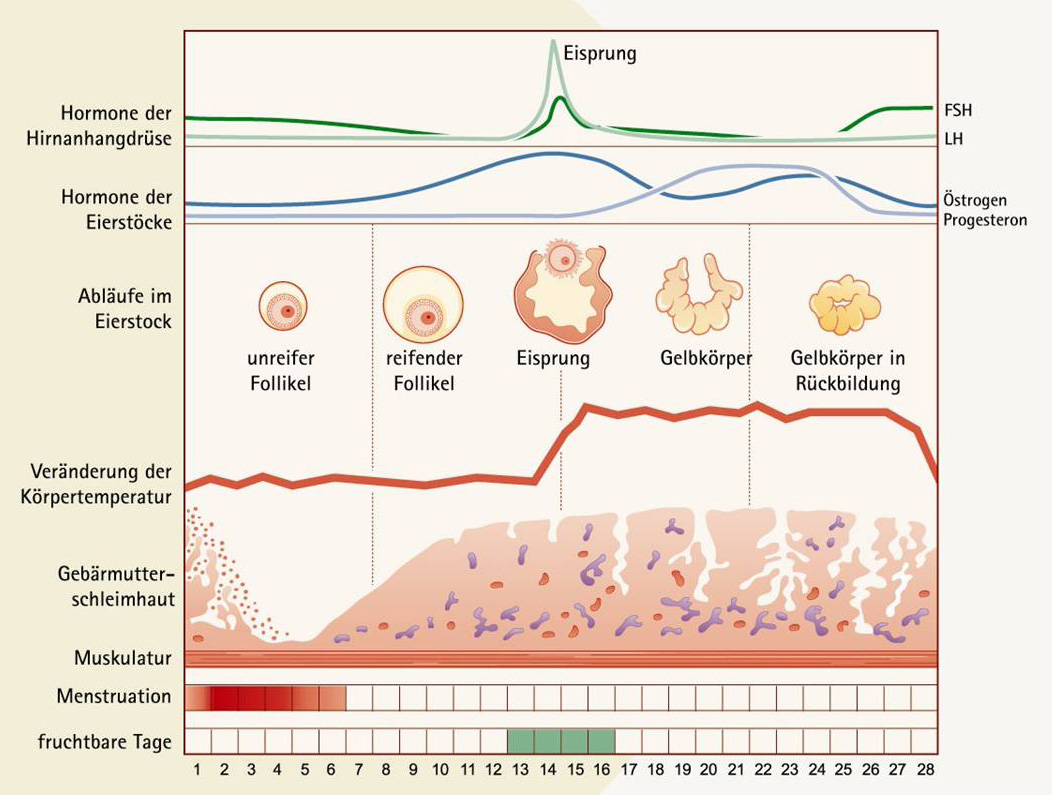
For this purpose, an ultrasound examination (vaginal) is performed on the 10th cycle day. The follicles on the right and left ovaries and the thickness oft he endometrium are measured. Usually, only one larger follicle is seen. If this is not yet large enough, it is checked again after two days. A ripe follicle measures about 20mm. Often a number of smaller follicles (around 10mm) can be seen at the same time. If a larger follicle is present, a blood sample is taken to determine E2 (estradiol) and LH (Luteinizing hormone). The estradiol correlates with the maturity of the egg and the LH surge causes ovulation. An optimal case would be the detection of an 18-22mm follicle at mid-cycle with adequate estradiol and LH levels. There are variations from cycle to cycle, however if you have no follicle growth over multiple cycles, we will recommend hormone stimulation.

DNA Fragmentation Test
/in DNA Fragmentation Test_en/by econsorA variety of factors can lead to strand breaks (fragmentations) in the DNA of sperm. With the help of the DNA fragmentation test (halosperm test), your sperm can be examined for DNA damage by using a special staining method. During the procedure, the sperm are treated and stained so that the chromosomal DNA unfolds and wraps around the sperm head in the form of loops (a halo). In sperm with fragmented, i.e. broken DNA, these loops do not form or only form very
weakly. Therefore, no halo is seen.
The most important factor to be taken into account from this test, is the „DNA Fragmentation Index“ (DFI). The higher this index, the lower the probability of natural fertilization and thus pregnancy and birth. The result provides the doctor detailed information about sperm quality, and supports selection of the appropriate treatment method (insemination, IVF or ICSI).

Gemeinschaftspraxis
Gynäkologische Endokrinologie
und Reproduktionsmedizin
Hagellocher Weg 63
72070 Tübingen
Telefon 0 70 71 94 663-0
Mobil 0172 776 21 67 (Nur in Notfällen)
Fax 0 70 71 94 663-99